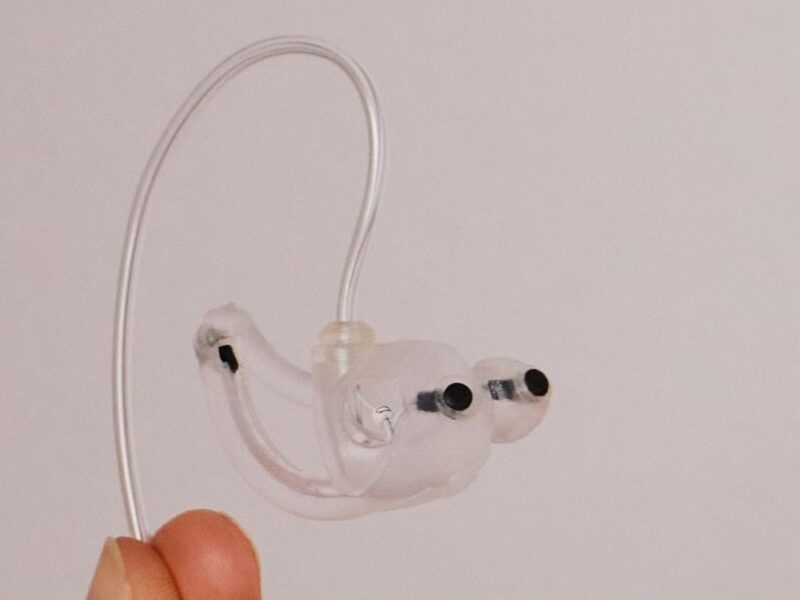
Measuring EEG through the ears to screen for dementia
 Cette publication existe aussi en Français
Cette publication existe aussi en Français
Aarhus University has teamed up with T&W Engineering, a Danish health technology firm, to create and evaluate an EEG sensor that fits in the ear.
The DKK 26m (€3.5m) Progression Assessment in Neurodegenerative Disorders of Ageing (PANDA) project will develop a custom-built measuring tool to be tested on groups of patients, including those with and without Alzheimer’s and Parkinson’s disease. The objective is to investigate whether the technology can be used to conduct screenings for these two severe brain ailments.
The ear-EEG records the electrical activity in the brain and maps sleep patterns in a non-invasive manner. Current research indicates that a person’s sleep patterns can reveal early indications of Alzheimer’s and Parkinson’s disease, conditions that gradually develop over many years. Patients typically only receive a diagnosis once they start experiencing cognitive and memory-related issues, sleep disruptions, or musculoskeletal system problems. By that time, treatment options are limited to symptom management.
The four year project aims to identify indications of these two ailments 10-15 years before the initial symptoms appear, says Professor Preben Kidmose, who leads the Centre for Ear-EEG at Aarhus University.
T&W Engineering is responsible for integrating the various sensors into the ear-EEG via a custom ASIC and developing the diagnostic support system for clinical trials, while Aarhus University is responsible for developing the biomarker algorithms for dementia.
The ear-EEG device is inserted into the ear to detect electrical activity in the brain. The technique records minute voltage fluctuations on the skin’s surface caused by the neurons’ electrical activity in the brain. It is a less invasive and more comfortable method than conventional sleep monitoring techniques.
The device also includes an oximeter to measure the oxygen levels in the blood, a thermometer, and a microphone that can detect breathing and heartbeat sounds, similar to a stethoscope.
The objective is to make the technology user-friendly so that patients can use it comfortably at home for an extended period. Ideally, individuals could monitor their sleep patterns over several days, weeks, or months every year to identify any changes that could be early signs of severe brain diseases, including Alzheimer’s and Parkinson’s disease. This would enable earlier and easier diagnoses, providing a significant advantage for patients.
international.au.dk/; www.tweng.com/
 If you enjoyed this article, you will like the following ones: don't miss them by subscribing to :
eeNews on Google News
If you enjoyed this article, you will like the following ones: don't miss them by subscribing to :
eeNews on Google News



